Cartilage damage
The bone in the knee joint is covered with a smooth layer of cartilage, which allows the knee joint to move freely. This layer of cartilage is approximately 5 mm thick and ensures even distribution of pressure and impact forces. There are no nerves in the layer of cartilage, and it stops growing after puberty.
A cartilage damage can be caused by wear and tear, chronic incorrect exertion or an accident (trauma).
Quick facts
-
Causes: A cartilage damage can be caused by wear and tear, chronic incorrect exertion or an accident (trauma).
-
Symptoms: start-up pain, pain with certain types of exertion, unstability, inflammation, swelling
-
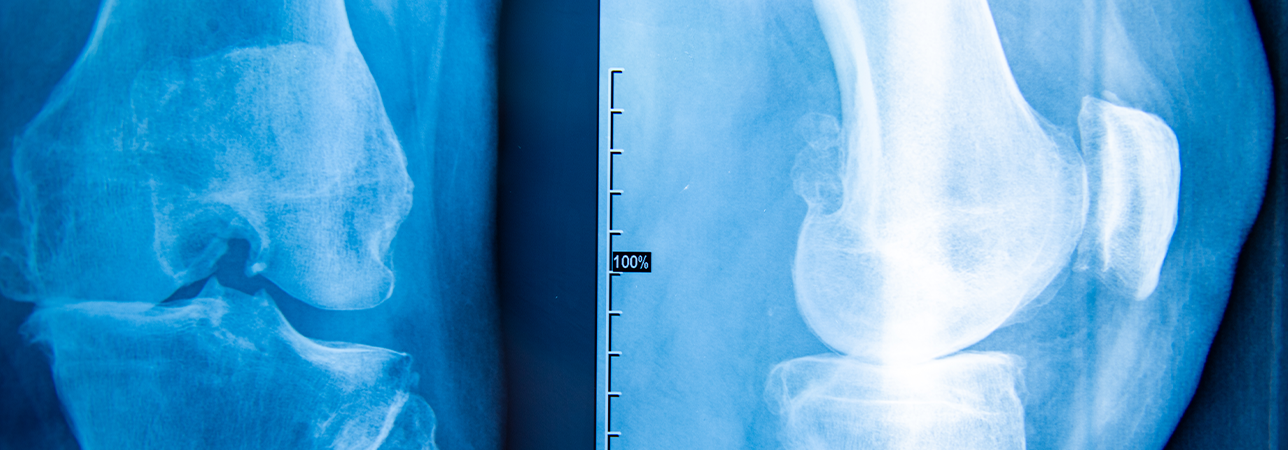
Diagnosis: To diagnose cartilage damage, the knee joint is X-rayed and an MRI scan of the knee joint is taken. In order to rule out further injuries or to determine the position of the leg axis, further investigations may be carried out.
-
Treatment: How cartilage damage is treated depends on its cause. Both conservative and surgical treatments, including a prosthesis, are possible.
Causes
Over the years, cartilage wears down and loses its ability to store water. As a result, the cartilage surface becomes brittle and develops cracks.
This brittle surface is more susceptible to impact and shearing forces. Because the cartilage does not contain nerve fibres that detect pain, we do not feel this change when it first occurs.
The articular cartilage can also be damaged by chronic incorrect exertion or an accident (trauma).
Diagnosis
To diagnose cartilage damage, the knee joint is X-rayed and an MRI scan of the knee joint is taken. In order to rule out further injuries or to determine the position of the leg axis, further investigations may be carried out.
The rotation of the knee joint is determined using a rotational CT scan.
The results of the investigations are analysed in close detail. Cartilage damage can only be treated effectively if existing clinical pictures are eliminated, such as lateral deviation of the patella.
Symptomatic cartilage damage in young patients should be treated surgically in order to prevent or at least slow down the progression of osteoarthritis in the knee, as well as to allow the patient to resume pain-free physical activity.
Stages of cartilage damage

Damage to the articular cartilage may consist of small tears on the surface, but it can also affect the entire cartilage in the knee. This exposes the rough, painful surface of the bone.
Cartilage damage is divided into four stages:
- Stage 1: soft cartilage
- Stage 2: rough surface with cracks
- Stage 3: deep cracks in the cartilage that go to the bone
- Stage 4: complete deterioration of cartilage with exposed bone
Treatments
How cartilage damage is treated depends on its cause. Before the intervention, a distinction is made as to whether the damage has been caused by wear and tear (chronic) or as a result of an accident (acute).
Conservative therapies
As the cartilage only continues to grow until puberty and therefore loses its capacity for self-regeneration, the possibilities of conservative therapy are quite limited and the condition can only be alleviated by trying to slow down its progress with special therapies.
In the case of cartilage damage, it is important to be conscious of how much you weigh. In some cases, it may be necessary to lose weight. The development of cartilage damage can be slowed down by regular exercise with steady movements, such as swimming or cycling.
Surgical treatment
Which surgical therapy is used depends on the extent and depth of the cartilage damage. The age of the patient, the condition of the exposed bone and the quality of the cartilage are also taken into account.
Cartilage treatment using the body’s own cartilage tissue
In this surgical procedure, the body’s own cartilage tissue is used to treat the cartilage damage. This minimally invasive procedure is carried out as an arthroscopy (joint endoscopy). During the procedure, healthy cartilage is removed from the knee. The cartilage from the different areas is mixed with a fibrin glue (thrombin). This creates a viscous mass, which is used to fill the damaged cartilage. The filled area is then mixed with particles from your own blood. This activates the cartilage and supports the formation of new cartilage.
Aftercare
The type of aftercare is determined according to the treatment the patient has undergone.
If the cartilage has been treated surgically, the patient must not bear weight on the knee joint for six weeks. In this case, the patient will use crutches.
Immediately after the operation, the knee joint is immobilised using a special splint. This will be worn for two days. After that, the splint is only worn at night for six weeks.
As the knee joint can only be bent a maximum of 30° in the first 14 days after the operation, an orthosis is used during the day. Over the next six weeks, the patient can begin to gradually increase the flexion of the knee – from 60° to 90°. During this time, walking is only allowed while using crutches.
If the patient has undergone resurfacing, the knee joint can bear weight and be moved from day one. To protect the new joint, it is recommended that crutches are used for the first few weeks. The most important part of the aftercare is several weeks of intensive physiotherapy to strengthen the thigh muscles.
FAQs
Can a cartilage tear heal by itself?
The layer of cartilage it stops growing after puberty. Damage is irreversible. If left untreated, cartilage damage leads to osteoarthritis over time.
How long will I be out of action following cartilage damage?
If the cartilage has been treated surgically, the patient must not bear weight on the knee joint for six weeks. In this case, the patient will use crutches.
What are lubricant injections?
Hyaluronic acid injections are used to temporarily improve the lubrication of the defective joint. This reduces the inflammation in the joint and thus alleviates pain. Another option is to inject the joint with the patient’s own blood.